Solutions & treatments
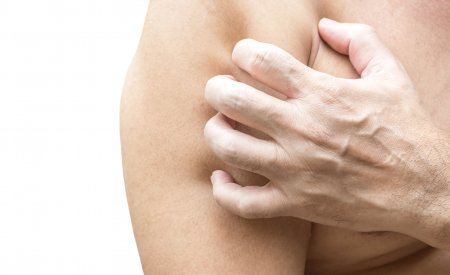
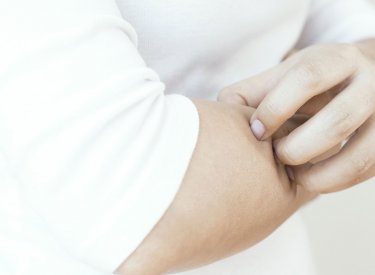
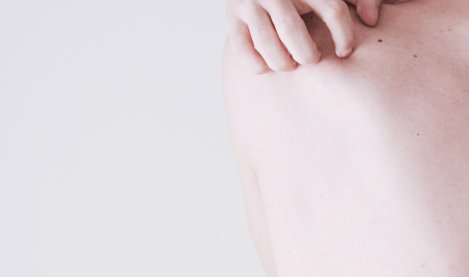
What happens in atopic skin? (and how can you reduce eczema flare-ups?)
A more severe form of very dry skin, irritated skin with itching is considered atopic skin. This skin disease starts at a very young age and has all the characteristics of a genuine epidemic. It is even one of the main causes of visits to the dermatologist! In the past 30 years, the number of cases of atopic dermatitis has doubled or even tripled in western countries*.
Atopic skin is not well known or understood, yet it disrupts the lives of children and their parents. However, recent scientific discoveries have improved understanding of the illness and changed the way it is treated starting at birth.